After a busy week in the office, I was enjoying my morning coffee on Fire Island when I received an “emergency” phone call from my patient, Tina.
Tina had been the recipient of extensive restorative dentistry (crowns and permanent bridgework) over the course of her adult life. She is now 68 years old with failing dentistry: decay under her crowns and bone loss due to periodontal/gum disease.
As a new patient to my practice, I spent a good deal of time with Tina evaluating her current condition and discussing with her in great depth the treatment choices she had to address her immediate needs and fulfill her desire to keep her smile, avoid dentures, and keep the cost of care within her means.
We decided upon a course of treatment that would span approximately two years. Most of that time was to be passively spent living her life while her bone was maturing or her dental implants were integrating. In other words, the two years time frame was not actually two years of active treatment in my office. Tina would spend most of those months living her life without dental appointments, except for periodic cleaning and examination.
So, we decided upon a treatment plan that included yesterday’s three and a half-hour appointment during which I surgically placed the implants accompanied by a fairly large bone graft in the adjacent area. Although Tina had sufficient bone to place the implants, I reinforced the existing supporting bone with more volume to ensure long-term success.
Tina hadn’t had implant surgery before and was a bit apprehensive. But everything went very well and she left my office with a smile – albeit a lopsided one from the local anesthetic. My staff made sure she was equipped with all the necessary post-op accoutrements including antibiotics, pain medication, instructions and, of course, my cell phone number.
So, when Tina called I was, of course, concerned. She beat me to the punch because I was going to call her later that morning.
“Dr. Sinkin,” she asked, “Is it normal that I don’t feel any pain?”
I couldn’t help but crack up. This was Tina’s emergency?
Here’s the story: Tina had heard from a number of her friends and colleagues that the recovery from implant surgery and bone grafting involved a lot of swelling and pain. She was concerned that something was wrong because she felt no pain! And had virtually no swelling.
I assured her that all was well and explained that some of the horror stories shared by her well-intentioned (yet under-informed) friends, were probably exaggerated. Some of the stories did not apply to her exact condition, some were hearsay hyperbole, and likely, a few involved unintended post-operative complications.
Tina’s surgery had gone well, she was aware of what was being done, why it was done, how it was done, and what to expect in the days to follow.
As we finished our conversation she once again expressed with incredulity how good she felt. Perhaps, I offered up with a smile on my face, it’s because I’m that good at what I do – or maybe we just got lucky! Now it was her turn to laugh.
Health information is empowering – but always consider the source. Make sure to ask your doctor what to expect. It’s in both of your best interests to know the facts and communicate realistic expectations.
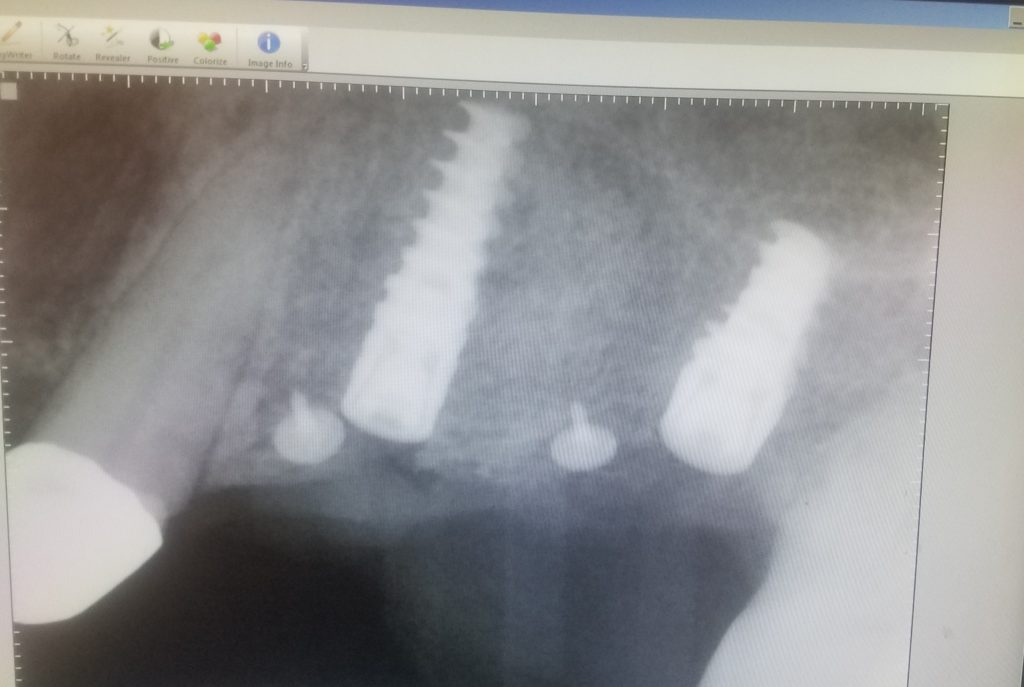
This x-ray is of the two implants I placed for Tina. The two white circular objects are bone tacks securing the bone graft in place.